|
8/30/2023 0 Comments Plexiform layers 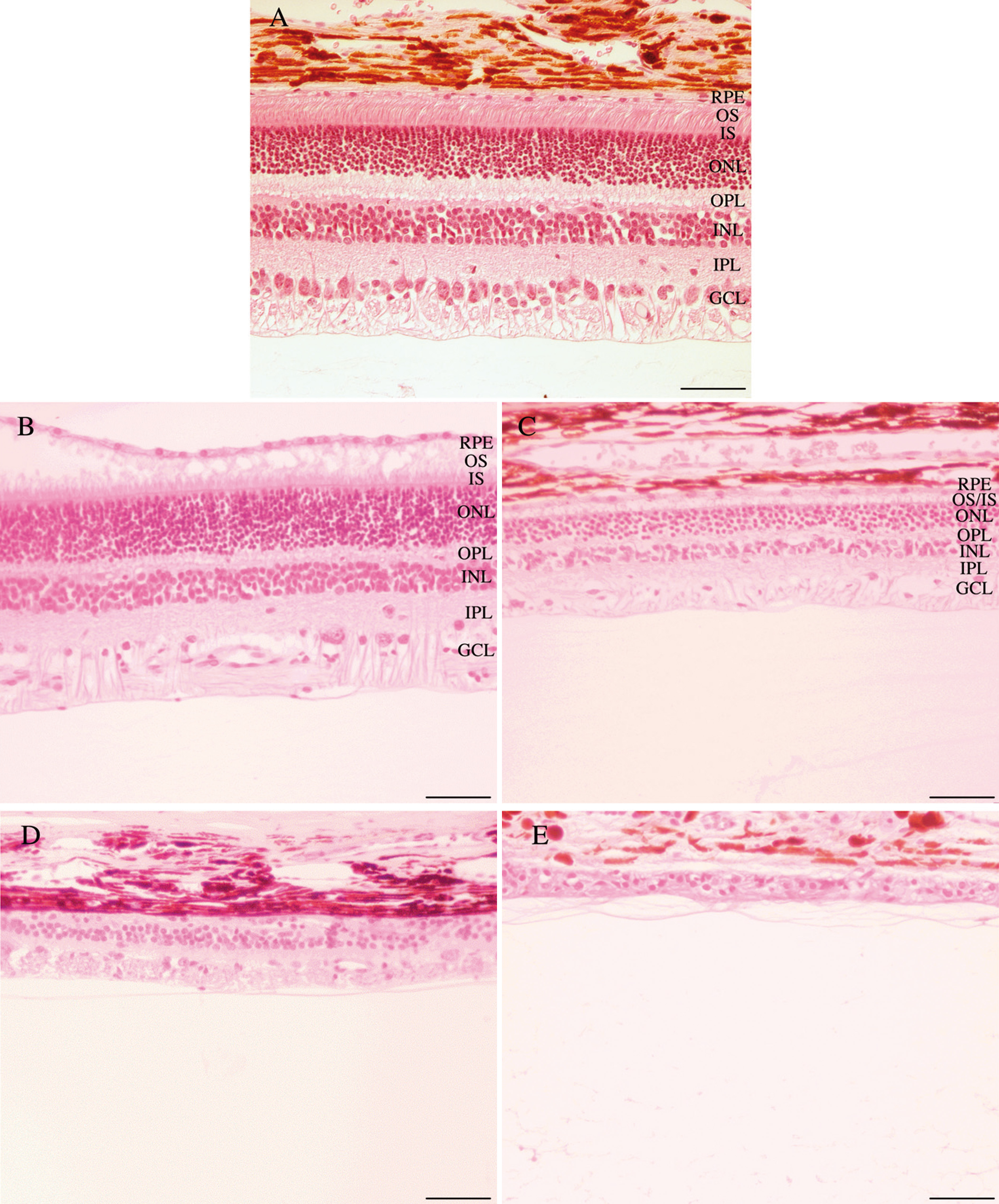
Combining GCC/GCIPL thickness, pRNFL thickness, ONH parameters, psychophysics examinations, and vasculature evaluations, though, can help to improve the overall glaucomatous diagnostic ability and accuracy. The thinning of macular ganglion cell layer (GCL) and peripapillary retinal nerve fiber layer (pRNFL) has been well recognized as biomarkers of optic nerve damage, which can be quantitatively measured by optical coherence tomography (OCT) in a non-invasive, precise, and reproducible way.Ī number of studies have showed that the macular ganglion cell complex (GCC, the sum of RNFL, GCL, and inner plexiform layer) thickness or the macular ganglion cell–inner plexiform layer (GCIPL) thickness has similar glaucoma discriminating performance with that of pRNFL. The human retina contains an estimate of more than 1 million RGCs, over 50% of which locate in the macular, making it the easiest region for calculating the RGC counts and detecting their loss. Īs the output neurons of the retina, RGCs are the only part of the central nervous system that can be optically detected in vivo. There may be a 20–40% of RGC loss prior to detectable visual field defect, indicating that evaluation of RGCs could be beneficial in detection and monitoring of glaucoma. Previous studies have showed that structural glaucomatous changes primarily affect RGCs and their axons, followed by functional changes featured by characteristic glaucomatous visual field defect. The hallmark of glaucoma is progressive loss of retinal ganglion cells (RGCs) in the inner retina and their axons in the optic nerve head (ONH). 
Glaucoma is one of the leading causes of irreversible blindness worldwide. This is relevant in comprehensively understanding the normative data and differentiating normal aging from abnormalities. Individual determinants associated with thinner GCIPL thickness were older age (particularly over 40 years of age), thinner pRNFL, and weaker OCT signal strength. There was no significant correlation between GCIPL thickness and SE, IOP, CCT, and AL ( P = 0.135–0.968). No significant difference was found between males and females ( P = 0.069–0.842), and between right eyes and the left eyes ( P = 0.160–0.875) except that of superonasal GCIPL thickness ( P < 0.001). Determinants of thinner GCIPL thickness were older age ( P = 0.001–0.117 effects enhanced if age over 40 years), thinner pRNFL (all P < 0.001), and weaker signal strength (all P < 0.001). The age, gender, laterality, spherical equivalent (SE) refractive error, intraocular pressure (IOP), axial length (AL), central cornea thickness (CCT), circumpapillary retinal nerve fibre layer (pRNFL) thickness and OCT signal strength were recorded and their respective effect on GCIPL thickness parameters were evaluated. GCIPL thickness were obtained using Cirrus high-definition optical coherence tomography (OCT). This was a retrospective study conducted on 225 normal eyes from 225 healthy Chinese adults. This study aimed to investigate the influences of multiple potential determinants of macular GCIPL thickness in normal Chinese adults. Demographic, systemic and ocular factors may impact macular ganglion cell–inner plexiform layer (GCIPL) thickness measurements. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
